To see if you have been exposed to the bacterium that causes Lyme disease
Lyme Disease Tests
If you show symptoms of Lyme disease, especially if they appear some weeks after a painless bite from a small tick or you have recently been in woodland or long grass
A blood sample taken from a vein in the arm
None
-
How is it used?
The first test done is an enzyme-linked immunosorbent assay (ELISA). The UK Health Protection Agency Lyme Borreliosis Unit uses one that detects both IgM and IgG antibodies to B. burgdorferi . The ELISA is sensitive but has a high false positive rate, giving positive results in glandular fever, rheumatoid arthritis and other autoimmune conditions.
If the ELISA is positive, an additional test called a Western blot is used to help your doctor confirm a diagnosis of Lyme disease. The UK Lyme Unit uses Western blots that test for IgM and IgG antibodies separately.
Another specific test, the polymerase chain reaction (PCR), detects the DNA of B. burgdorferi. It is used to confirm the presence of the bacterium in joint fluid in Lyme arthritis and in cerebrospinal fluid (CSF) in Lyme meningitis.
-
When is it requested?
Laboratory tests are unnecessary if you have had a tick bite that becomes red and swollen when the tick is still attached or shortly after it drops off or is removed, but disappears quickly and you have no other symptoms. This is a tick hypersensitivity reaction, not Lyme disease.
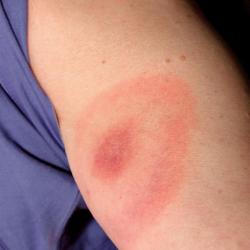
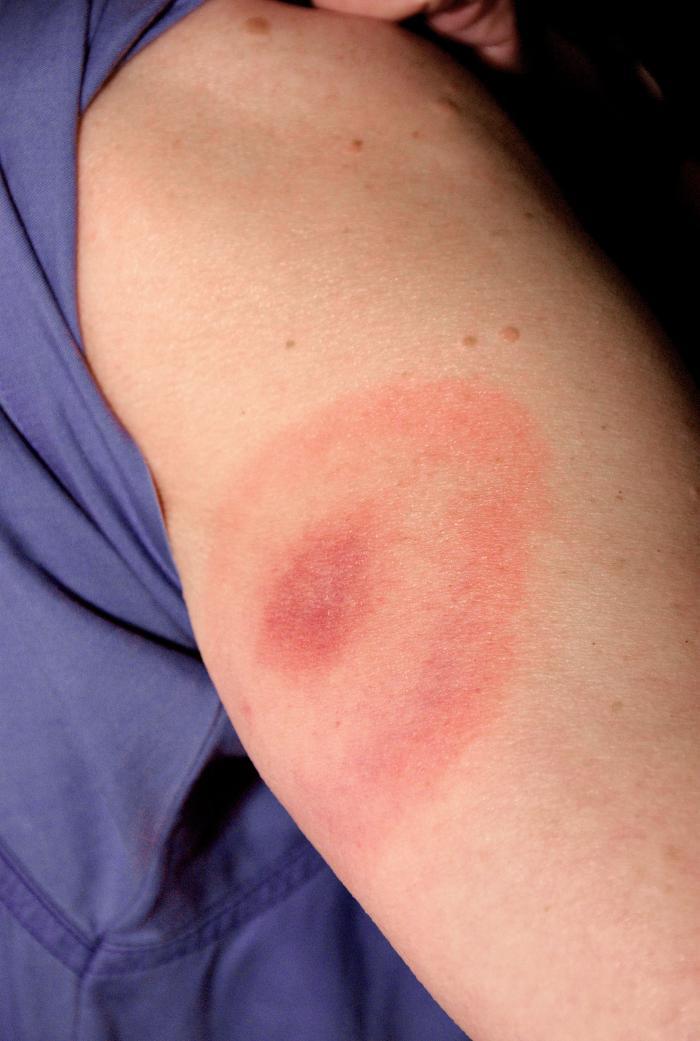
If you develop the characteristic spreading rash of Lyme disease (erythema migrans) 3 to 30 days after a tick bite or possible exposure to ticks, your GP is highly likely to make a clinical diagnosis. You will be treated with antibiotics without having had any laboratory tests, and should make a complete recovery.
However, if you see your GP without a characteristic rash but with other symptoms that occur in early or later Lyme disease blood tests may be requested, particularly if you say that you have had a recent tick bite or possible exposure to ticks in wooded or long grass areas.
-
What does the test result mean?
If the ELISA test is carried out within a few weeks of a tick bite or possible exposure it may fail to detect antibodies to B. burgdorferi, and will usually be repeated a few weeks later. About 30% of tests are positive by two weeks and about 80% by six weeks. The rate increases with duration of infection until more than 99% are positive.
If the ELISA test is positive and both the IgG and IgM Western blot tests are negative, it is probable that the ELISA result is a false positive and Lyme disease is not the cause of the symptoms.
If the ELISA and IgM tests are positive, with or without a positive IgG test, early Lyme disease is probable and treatment with antibiotics is advisable.
A positive ELISA test with a positive IgG and a negative IgM test can be seen in later Lyme disease. However, it should be born in mind that these results can also be seen when exposure to B. Burgdorferi took place a long time ago, and the current symptoms may be unrelated. This is particularly likely in people who have been exposed to tick bites at work (like foresters), during recreation (like ramblers) or because they live near woodlands or heaths.
-
Is there anything else I should know?
-
What can I do to prevent infection?
There is no vaccine to prevent Lyme disease, so it is important to take precautions to reduce the risk of becoming infected when going to wooded or grassy areas, particularly in the spring and early summer. When on holiday, remember that the risk is greater in other European countries and in the US than in the UK.
Wear a long-sleeved top and tuck your trousers into your socks. Ticks are easier to spot if your clothing is a light colour. Use an insect repellent. At the end of the day inspect your skin and that of your children for ticks, particularly the scalp, armpits, groin, back of the knees and the waist band area. Remember to check any pet, too.
To remove a tick, carefully grasp it gently by the head part (not the body) as near your skin as possible, preferably with fine-toothed pointed tweezers, and lift it straight out. If you have been bitten, don’t become over anxious: only a minority of ticks in the UK are infected, and only those infected that are left on the skin for more than a day are likely to pass on the infection. However, if a spreading rash or symptoms of flu appear in two to four weeks, see you GP straight away.
-
What is the Post-Treatment Lyme Disease Syndrome?
A small proportion of people treated for Lyme disease with the recommended 2-4 week course of antibiotics have symptoms, including fatigue and joint and muscle pain, that persist sometimes for more than 6 months. Research is ongoing to better understand the cause of this syndrome. People should contact their GP if symptoms persist. There is early evidence that further antibiotic treatment may be helpful.